Winter is rapidly approaching and for many of you it’s already cold and the nights getting longer. With this brings increased odds of getting sick, getting depressed and getting fat. None of these things any of us want, but it’s sort of taken as a given in the winter time. Well, a couple years ago, I got really fed up with just accepting this as a reality and I figured there had to be a way to mitigate this outcome. Seemingly, all roads led back to vitamin D.
What I found in my research is not only that we need to be taking more vitamin D in the winter—a trivial realization, but more specifically that we’re not only supposed to be taking vitamin D, but massive doses of vitamin D relative to conventional wisdom. Now, I’m going to preface this article with a couple of things. One, I am not a doctor and I do not claim to be and two all of these conclusions that I am coming to are based upon my own research and experimentation. You are free to disagree. However, I am only writing this article because I have done—and am currently doing—what I’m going to present to you, and it works for me. I suggest that you do your own research in tandem and also slowly experiment if you like what I’ve compiled here because results may vary.
Do not sue me if something goes wrong. I am poor and you will get nothing but my manga collection out of the lawsuit.
With the disclaimer out of the way, let’s establish some background.
What Is Vitamin D?
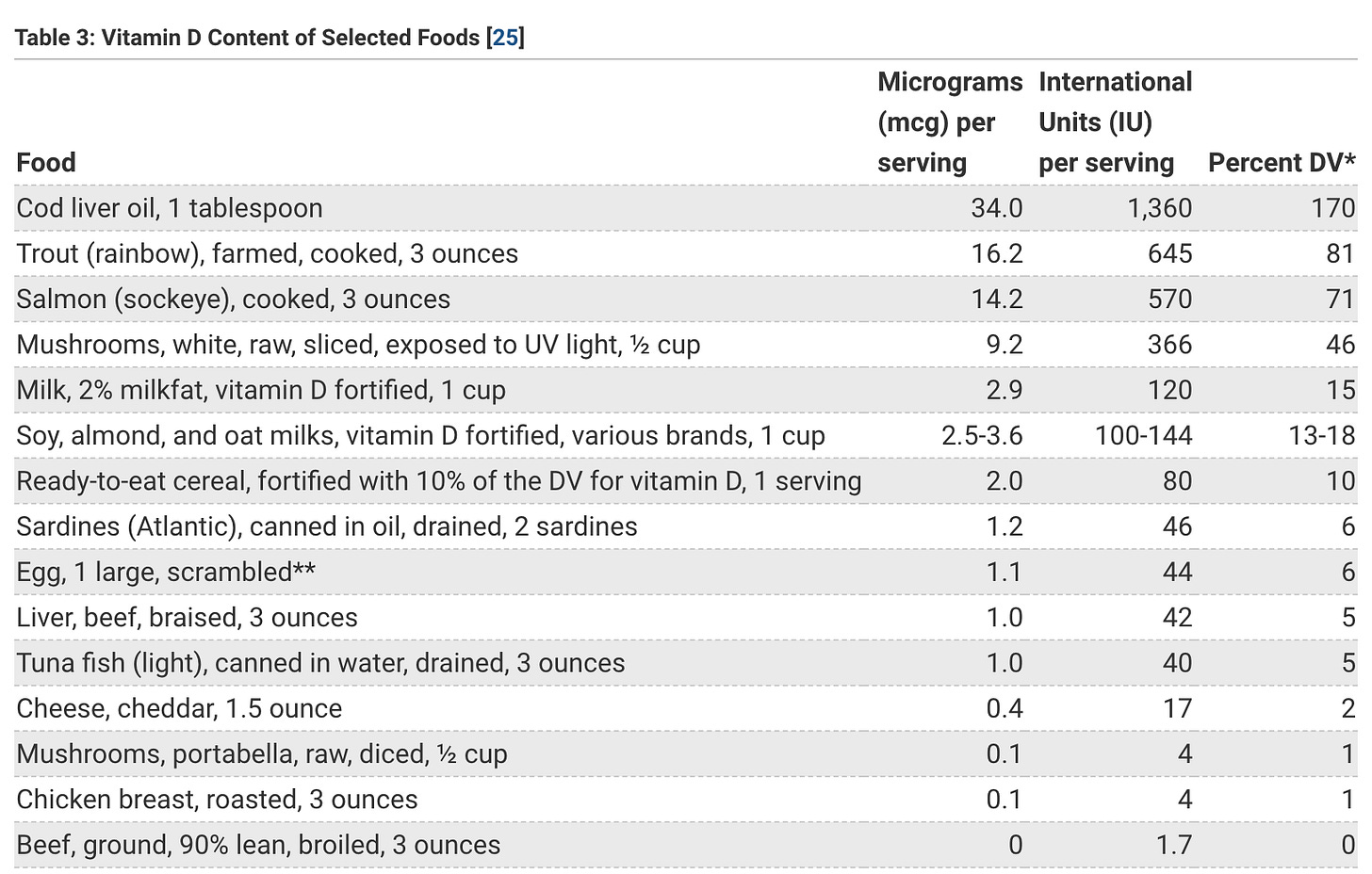
Even the layman ought to be able to tell you that vitamin D is a vitamin you largely receive from the Sun, but is also present in several foods. Well it’s not actually something you “receive” from the Sun. Your body produces vitamin D endogenously when it comes in contact with ultraviolet light from the Sun. Vitamin D obtained from sun exposure, foods, and supplements is biologically inert and must undergo two hydroxylations in the body for activation. This becomes important later, but you don’t need to necessarily understand the chemistry in depth.
“The first hydroxylation, which occurs in the liver, converts vitamin D to 25-hydroxyvitamin D [25(OH)D], also known as “calcidiol.” The second hydroxylation occurs primarily in the kidney and forms the physiologically active 1,25-dihydroxyvitamin D [1,25(OH)2D], also known as “calcitriol” (emphasis mine)
Vitamin D “promotes calcium absorption in the gut and maintains adequate serum calcium and phosphate concentrations to enable normal bone mineralization (NIH).” This in turn prevents bone related medical issues such as rickets and osteoporosis. Beyond simply your bones, vitamin D also aids in “reduction of inflammation as well as modulation of such processes as cell growth, neuromuscular and immune function, and glucose metabolism.” Essentially, vitamin D is pivotal in many of the processes that make the fundamental systems in your body function. It is fundamental in strengthening your immune system, handling how you put on or take off weight, and just how your body functions period. As these are critical systems, obviously you would want these running optimally at all times. If that’s the case, why is there such a fear around maximizing the strength of these systems?
When I tell the average person I’m taking megadoses of vitamin D they freak out or are quick to tell me it doesn’t work or it is going to make me very sick.
Whenever I encounter this kind of reaction from an idea that is seemingly innocuous, I always am tempted to look deeper. You’ve all experienced this, Im sure. During covid, if you mentioned Ivermectin or vitamin D or simply anything that CNN hadn’t reported yet, you were met with insane amounts of backlash. This is a strange social phenomenon. It’s the superego having an immune reaction to wrong think. Typically, when you encounter this, you can probably find something you’re not supposed to look into right beneath the surface.
This time, the heretical truth was:
You should be taking somewhere between 10,000-50,000 IU per day of vitamin D3.
The optimal dose seems to be about 30,000 IUs as noted by a few people in my research but results will vary.
Particularly, the dose will vary with your skin complexion and your geographical latitude. If you live somewhere like NYC, you should be taking 30k+ —especially in the winter. If you live somewhere like Los Angeles, you can probably take more like 10k and be just fine. Additionally, if you take those same geographical locations, but you’re fair skin, you can probably get away with 10k, but if you’re dark skin, you probably want a full 50k dose.
When I say this to people, the first thing I hear is that this is dangerous. Conventional wisdom dictates that this is far too high and you will be at risk for hypervitaminosis D i.e. hypercalcemia. A cursory look for the current recommendations for vitamin D intake from Harvard Health states (emphasis added is my own)
Based on the evidence for bone benefits, however, the IOM panel increased the RDA for vitamin D to 600 IU for people up to age 70 and to 800 IU for those over 70. That's a fairly sizable boost over the previous recommendations of 200 IU per day through age 50, 400 IU for ages 51 to 70, and 600 IU for ages over 70. The IOM also raised the safe upper limit of daily intake for most age groups from 2,000 to 4,000 IU.
The current recommended dose appears to be around 600IUs a day for the average person and slightly higher for senior citizens. The recommended upper limit is between 2-4k IU.
Why then am I so confident that not only you can take more than this, but you also ought to be taking and order of magnitude more?
There is a long complicated history with vitamin D and the medical/pharmaceutical establishment. As with most things in the health industry, there’s a lot of misinformation which has poisoned the well and we never quite recovered. Remember when we were told to eat 8-10 servings of grains a day? Remember when we were told eggs were bad for you? Remember when we were told you should stay away from fat and cholesterol in your food? The medical/health/pharmaceutical industry, like many, has competing lobbies and influential people involved making decisions to help their bottom line and they rarely update the public to keep pace with modern understanding.
If you look back at the above quote, you can see they increased the recommended dose from 200IU per day. The previous suggested dose was set that low for a reason. Let’s first address the history of our understanding of vitamin D to get a better understanding of where we are now.
Misconceptions Concerning Vitamin D
Back in the 1930s, many children were being diagnosed with rickets. This is a painful bone disease which was common among children living in smog covered industrial cities. The smog was blocking the Sun and after much experimenting they found a substance which cured rickets. Since this substance was found to cure rickets similar to the manner which vitamin C cured scurvy, scientists determined that this must also be a vitamin. The problem is, vitamin D is not a vitamin, it’s a hormone.
What makes something a vitamin is that it’s ingested in small quantities to promote bodily functions. However, unlike a vitamin, vitamin D is produced endogenously from UVB contact with our skin and is used to perform endocrine and autocrine function. This subtle misconception came with major consequences. Since this substance was considered to be a vitamin, it was given recommended dosage levels that a vitamin would have.
Since vitamin D is fat soluble, any vitamin D which is not used is absorbed into your body’s tissues. It was then concluded that similar to other fat soluble vitamins, if this build up was occurring, then it would prove toxic or dangerous. Therefore, the lowest dose that was effective in treating rickets, was all that anyone should ingest. The “safe dose” therefore this became the range of doses and anything above this range was approaching toxicity. This became the standard and was largely not questioned for many years, despite no trials ever being performed to confirm.
In fact, this is STILL the current blood serum levels which are considered approaching toxicity.
Vers, but it is very possible that you can come to a correct conclusion via incorrect thinking. What if this is correct despite their reasoning being flawed?
Yes, I’m glad you asked.
As it turns out, we already know with absolute certainty this chart is incorrect.
Although current data support the viewpoint that the biomarker plasma 25(OH)D concentration must rise above 750 nmol/L to produce vitamin D toxicity, the more prudent upper limit of 250 nmol/L might be retained to ensure a wide safety margin.
You see, in order to avoid potential accidents for the public, they knew that you cannot get toxicity below 750 nmol/L of vitamin D3 (which converts to 300 ng/mL) , but they determined they should make it medically public that 250 nmol/L of vitamin D3 (i.e. 100 ng/mL) is the limit for toxicity as a “margin for error.” They wanted public facing products and recommendation to be significantly lower because the average consumer is kind of an idiot. There’s a million stories of people taking an entire bottle of Tylenol (i.e. acetaminophin) for a headache, then ending up in the hospital with acute liver failure. So making the public-facing upper limit three times lower than the actual lower limit seems to them like a wide enough berth to avoid litiga—I mean accidents.
It’s important to note in this case that what is being charted here is the serum blood levels of vitamin D. This doesn’t directly convert to the amount of any individual dose you ought to be taking. This refers to the amount present in your blood stream after the dose has been metabolized. More on this later.
The vitamin D misinformation problem is made worse because there is a major issue when it comes to supplement regulation in the US. There basically is none whatsoever. For this reason, there are many products which say they are X and in reality they’re 30% X and tons of fillers. Better yet, they’re really X’ a derivative of X or they’re actually X2 some alternative version of X. For this reason, it’s very important as a consumer that you read reviews and do your research when it comes to products.
This applies to vitamin D research because the vast majority of studies were done based on information we had about vitamin D from the early part of the 20th century when we largely knew nothing about it nor its pathways in the body. The most common version of vitamin D on the market was D2 (Ergocalciferol), which we now understand is metabolized completely differently within the body than vitamin D3 (Cholecalciferol) which studies confirm
Despite an emerging body of evidence suggesting several plausible explanations for the greater bioefficacy of vitamin D3, the form of vitamin D used in major preparations of prescriptions in North America is vitamin D2.
The study goes on to conclude:
Vitamin D2, if given in high enough doses, prevents infantile rickets and is capable of healing adult osteomalacia. However, the inefficiency of vitamin D2 compared with vitamin D3, on a per mole basis, at increasing 25(OH)D is now well documented, and no successful clinical trials to date have shown that vitamin D2 prevents fractures.”
If you take a deep dive into the references in the above study (which I recommend btw), an image starts to come into focus. For a long time, the distinction between D2 and D3 wasn’t well understood. It appears that different age groups metabolize D2 differently. Additionally, the synthesis of vitamin D is done in two different ways for D2 and D3.
Synthetic production of vitamin D3 is manufactured in a similar manner to that which occurs naturally in human and animal skin, via the production of 7-dehydrocholesterol from cholesterol and subsequent irradiation to its active D3 form. Conversely, vitamin D2 is synthetically produced from irradiation of ergosterol derived from the mold ergot
The production of D3 more closely mirrors that found in humans and is not only processed better within humans, D3 also more shelf stable than vitamin D2. The D2 supplements often has massive irregularities in the stated dosage and the actual dosage due to this. There are several people who believe many of the negative side effects experienced by people who took D2 supplements may have been caused specifically by the instability of Ergocalciferol.
The basis for setting the threshold that low was specifically to avoid hypervitaminosis D i.e. hypercalcemia.
Excessive levels of vitamin D leads to high levels of calcium in the blood. As we mentioned earlier, it’s pivotal in the strengthening of bones. Too much and now calcium is being left in your blood. The major study which the fear of hypercalcemia comes from a study from the Kashmir Valley where patients were dosed with high doses of vit D and all got hypercalcemia.
All the patients had demonstrable hypercalcemia and vitamin D levels were high in nine of the 10 cases. The patients had received high doses of vitamin D and no other cause of hypercalcemia was identified
The part that uhhh often is not referenced comes a bit later when the author states "the patients were dosed with 3.6 million to 210 million IUs of vitamin D for a period of 1-4 months (median: 2). LOL
So you would imagine this insane dosage would have killed them right? Nope. 9 out of 10 of these patients survived and made a full recovery. The remaining one died from sepsis, not hypercalcemia. Oh and to make things better, this clinic actually had hundreds of patients and only these ten had hypercalcemia and they were taking 100 times the recommended dose of vitamin D.
Right now we have two extremes to work with for our (i.e. mine, fr don’t sue me) experimentation. We know that 600IUs is too low and 3,600,000 IU is too high. Seems like I can find a sweet spot.
Well I will save you all the trouble and tell you, that another study done at a hospital with 4700 patients has determined that doses between 5000 and 50,000 are perfectly safe for daily use and not one of the patients experienced hypercalcemia
During this time, we have admitted over 4700 patients, the vast majority of whom agreed to supplementation with either 5000 or 10,000 IUs/day. Due to disease concerns, a few agreed to larger amounts, ranging from 20,000 to 50,000 IUs/day. There have been no cases of vitamin D3 induced hypercalcemia or any adverse events attributable to vitamin D3 supplementation in any patient.
Great, so at the very least we know that we can operate in that range and have nothing to worry about in all likelihood. Since we now have a range of vitamin D to work with that we can assume to be safe. Let’s consider ways to narrow in on what doses work best for whom.
Just for safe measure, since we know that the major consequence of excessive vitamin D in your blood stream is hypercalcemia, we can further mitigate the extremely low chance of this by taking an additional supplement of vitamin K2 mk7. Conventional wisdom is, for every 10,000IU of vitamin D3, you take 100mcg of K2 mk7. Vitamin K2 regulates the calcium transfer within your body and makes sure that you wont end up with too much calcium in your blood. It will simply utilize the excess calcium where its needed.
edit: so to avoid the backlash from the
Vitamin D, Race and Schizophrenia
Keep reading with a 7-day free trial
Subscribe to version_4::samizdat to keep reading this post and get 7 days of free access to the full post archives.